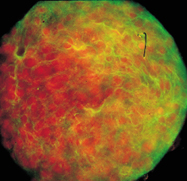
 Brain
Marrow
Brain
MarrowUF Research Opens New Windows
On Potential OF Adult Stem Cells
BY VICTORIA WHITE
|
|
 Brain
Marrow
Brain
Marrow
UF Research Opens New Windows
On Potential OF Adult Stem Cells
BY VICTORIA WHITE
Since the discovery
of their unique restorative properties, stem cells have been touted as
miracle makers, offering a possible cure for everything from Alzheimer's
to cancer.
But are they up to the challenge? And is there a source for them other
than embryonic tissue and all the ethical baggage it carries?
Dennis Steindler is staking his career on it. Steindler and his colleagues
at the University of Florida are pioneers in the discovery and use of
adult brain stem cells to achieve many of the same results as their more
controversial cousins.
He is optimistic that, like stem cells taken from embryos, adult stem
cells can be coaxed into supplying the right material for the job at hand,
whether it's repairing injured brains or spinal cords or providing healthy
cells to replace diseased ones.
"These adult tissues don't appear to be as restricted in their fate
as we once thought they were," says Steindler, a professor of neuroscience
and neurosurgery at UF's College of Medicine who also is affiliated with
UF's McKnight Brain Institute and the UF Shands Cancer Center.

"In some ways, they may not have the same potential as embryonic
cells, but once we figure out their molecular genetics, we should be able
to coax them into becoming almost anything we want them to be," he
adds.
Douglas K. Anderson, chair of UF's Department of Neuroscience and a key
player in UF's efforts to understand the biological response to spinal
cord injury, says of the Steindler team: "What makes them so unique
is their focus on adult tissues. They can take stem cells from cadavers,
obviating the need for having to deal with the controversies associated
with embryonic tissue. They've also shown that they can get stem cells
by 'dedifferentiating' them, a way of essentially turning old cells young
again."
Recruited en masse this year from the University of Tennessee, the Steindler
laboratory group includes eight experts in such techniques as identifying
stem cells and then multiplying their numbers in culture, exploring the
"DNA fingerprint" of stem cells and investigating a possible
connection between stem cells and uncontrolled tumor growth.
The lab complements the expertise of existing faculty who are studying
such cells in bone marrow, liver, pancreas and other parts of the body.
"There is a critical mass of highly skilled investigators here,"
says Steindler, explaining what drew him to his new lab, which occupies
more than 2,000 square feet of space within the state-of-the-art McKnight
Brain Institute. "The growing stem cell program here is one of the
most unique I have seen in the whole world."
Off campus, at the UF-affiliated Sid Martin Biotechnology Institute, Steindler
and his partner, Valery Kukekov, are involved in a startup company called
NeuroStem, which is seeking to attract corporate partners to support research
that will help move concepts uncovered in the academic laboratory into
the marketplace.
"From my perspective, the right cell for clinical use isn't there
just yet," he says. "Controlling the fate of the stem cell to
do what you want it to do is a daunting task. There's still a lot of biology
to be done on that. We also need to develop methods for expanding the
population of stem cells available for therapies."
While he believes that clinical trials will be coming soon to test adult
stem cells as a therapy
in people, he said it's important to continue the basic science research
in petri dishes and animal models to provide a solid foundation for such
experiments.
"It's extremely important for the continuing research that the therapeutics don't get tried before it's time or tried in an inappropriate manner," Steindler says. "That could lead to a worst-case scenario that will hurt the patient and will be terrible for the field because there would soon be cries to stop the research."
Molecular
Manufacturers
Ever stopped to wonder how the union of egg and sperm gives rise to the
development of a fully formed human being? Most people are satisfied with
a vague explanation of genes  providing
the blueprint and cells dividing repeatedly until a new person is ready
for debut.
providing
the blueprint and cells dividing repeatedly until a new person is ready
for debut.
Biologists seek much more precise answers. Their inquisitiveness led to
the discovery of what have come to be known as stem cells, which refers
to their ability to spawn not just mere copies of themselves but a variety
of other cell types. Embryonic stem cells can generate virtually all of
the body's tissue types. That's why they are so prized by researchers,
though the source of the cells remains a highly charged topic.
"Adult" stem cells, on the other hand, are those found in an
already developed tissue or organ. Their job is to create all of the cell
types within that particular locale. Thus, neural stem cells can give
rise to the three main types of cell of the brain - neurons, astrocytes
and oligodendrocytes.
Only within the past decade have scientists recognized that brain stem
cells exist beyond infancy.
"We are interested in how molecules that you see present in the developing
brain are involved in making it regenerative and resilient to injury,
at least compared to  the
aged brain," Steindler says.
the
aged brain," Steindler says.
They discovered that a family of proteins that was present while the brain
was developing disappeared by the age of 2 or 3. Eric Laywell, then a
graduate student in Steindler's lab and now a UF research assistant professor,
discovered that these proteins were present again near the site of an
injury in an adult brain.
"We figured that maybe the injured adult brain was trying to recapitulate
the events present during development, that it was trying to facilitate
brain regeneration," Steindler says. "That idea was kind of
heretical. Then we also started seeing new cells being born in a particular
region of the brain. That was rather shocking. That shouldn't have been
happening."
Steindler dubbed the source of the new cells "brain marrow"
to draw attention to its similarities to bone marrow, home to stem cells
that continuously replenish the variety of blood cell types the body needs.
Using tissue removed during surgery for intractable epilepsy, Kukekov,
Steindler and their colleagues were the first to demonstrate that they
could isolate a stem cell from the human brain. Before that, such cells
had been cloned only from rodents.
Two years ago, Laywell and Kukekov, now a UF research associate professor,
showed that they could isolate living stem cells from adult cadaver brains.
"That gave us the possibility for archiving these tissues, with the
goal of developing cell therapeutics for diseases and injuries, including
Alzheimer's, Parkinson's, multiple sclerosis, traumatic brain injury and
spinal cord injury," Steindler says. "And then the next earthshaking
finding was when Eric Laywell showed that you could take completely differentiated
adult cells and dedifferentiate them or turn them into young cells."
That, Laywell says, may play an important role in developing treatments
down the line.
"It's not a trivial procedure to get at the ventricles of the brain,
where the stem cells can be found," Laywell says. "It would
be much easier to get tissue from other regions of the brain and then
dedifferentiate it and turn it into stem cells."
One unique angle being explored by the UF researchers is whether there
is such a thing as a brain stem cell gone bad. Tatyana Ignatova, with
a background of 35 years of cancer research in Russia and the United States,
is spearheading that effort as a way to understand tumors called astrocytomas
and gliomas. In their high-grade form, these tumors are completely resistant
to treatment, typically regrowing quickly after efforts to eradicate them.
Ignatova, with assistance from her husband, Kukekov, and other lab members,
is finding intriguing evidence that these tumors may be sustained by a
small population of abnormal stem cells. One clue to the stem cell connection
is that the tumors display markers of neurons, not simply the markers
of astrocyte or glial cells - the type of brain cells from which they
are thought to arise.
"We've been able to see that the genes that are specific for neurons
are expressed in a glioma, which is not supposed to be, but there they
are," she says.
The stem cell connection may explain in part why the tumors are so difficult
to demolish.
"Cells during development must be very resistant to being killed
because otherwise there will be no development," Ignatova says. "They
are predisposed to develop."
By understanding these cells, Ignatova hopes to find the vulnerabilities
of the tumor cells.
Crazy
Ideas
Stem cell research has received so much publicity in recent months that
Steindler and his colleagues find it a bit jarring to think of a time
just a few years back when the number of scientists interested in the
field was tiny.
"When we were starting this, there weren't many labs working on these
ideas, so we would get our papers peer-reviewed by people who thought
we were crazy," Steindler says. "Our papers would fall into
the hands of people who thought we were from another planet."
But their ideas have held up through the years, replicated by other leading
laboratories or independently discovered at about the same time.
Today, the UF lab is one of about a half dozen in the world studying brain
stem cells with a high degree of expertise. Among the others are labs
at the National Institutes of Health, the University of California at
San Francisco, the University of Wisconsin, Cornell University and the
Salk Institute in La Jolla, Calif.
"We've been teaching students of biology and medicine for years that
nothing like this goes on," Steindler says, referring to the brain's
ability to generate new cells and the finding that the differentiation
time clock can run in reverse. "But guess what? We were wrong. It's
very exciting. By studying these cells and how to manipulate them, we
will be finding the cures for degenerative diseases, traumatic injuries
and cancer.
"We're learning that despite the aging process, we're far from useless.
We have the potential to repair and make new brain cells throughout life,"
he adds. "Because we have these cells in there, we can now talk about
preventing death or at least prolonging the quality of life by teaching
these cells to do more work than they're already doing."
Dennis A. Steindler
Professor, Departments of Neuroscience and Neurosurgery
(352) 294-0074
steindler@mbi.ufl.edu
Eric Laywell
Research Assistant Professor, Departments of Neuroscience and Neurosurgery
(352) 392-5658
elaywell@mbi.ufl.edu
Valery Kukekov
Research Associate Professor, Departments of Neuroscience and Neurosurgery
(352) 392-5955
vkukekov@mbi.ufl.edu
Tatyana Ignatova
Research Associate Professor, Departments of Neuroscience and Neurosurgery
(352) 392-5955
tignatova@mbi.ufl.edu