|
|
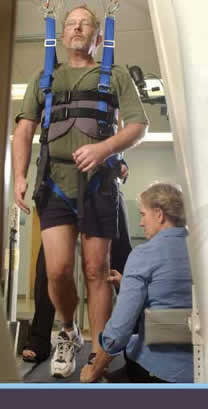
 UF's Brooks Center for Rehabilitation Research Draws on the University's Many Resources to Develop the Science of RehabilitionBy Jill Pease One moment, Paul Schauble was enjoying a bicycle ride. The next he was staring at the sky. Schauble, a professor and psychologist at the UF Counseling Center who was an avid mountain climber and cyclist, was riding in his Gainesville neighborhood in March 2001 when a dog darted into his path from between two parked cars. Schauble’s feet were strapped into the pedals and he flew over the handlebars as he braked. "I lay there stunned and kept trying to move and when I couldn't, I realized that I was paralyzed," Schauble says.Initially unable to move anything but his lips to speak, Schauble slowly regained some degree of sensation and motor function during weeks of hospitalization and rehabilitation therapy, but his ability to walk was severely limited. Schauble is just the kind of patient researchers at the University of Florida's Brooks Center for Rehabilitation Studies had in mind when they brought together the resources to build a comprehensive center to study and improve rehabilitation interventions, delivery and financing. "I am a collaborator, an essential member of the research team," Schauble says. "I'm invested in the outcome of the research and the knowledge it generates, not only for the benefits I experience directly but also for the welfare of individuals suffering from my condition who may experience future. The Brooks Center is the realization of a career dream, says Pamela Duncan, the center's director. "I think we're going to make a difference in people's recovery after injury or illness," Duncan says. "We're getting people to work and think together who before only thought about their own area of research." Duncan says researchers from several UF colleges, including medicine, nursing, public health and health professions, health and human performance, engineering, pharmacy and liberal arts and sciences are collaborating to develop the science of rehabilitation and ultimately improve rehabilitation practice. "With the assistance of deans and department chairs we are building a culture within the University of Florida that will help us gain recognition as a world-class leader in rehabilitation research," she says. The vision of J. Brooks Brown, M.D., founder and chairman of Jacksonville-based rehabilitation provider Brooks Health System, and Robert Frank, dean of UF's College of Public Health and Health Professions, the center was created in 1999 with a $2.5 million gift to the college from Brooks Health. The gift was eligible for state matching funds, raising the total to $5 million. "We recognized that our organizationwide support of applied research in the area of rehabilitation treatment could one day be of profound service to mankind," says Brown. "Taking medical treatment to this level of innovation can only result in improved outcomes for patients, better access to rehabilitation treatment and lower treatment costs." "One of the challenges in developing the Brooks Center has been answering the question 'Why do we need a rehab research center and what is its importance?'" Duncan says. "The answer is that rehabilitation research programs are just as complex as those for cancer and genetics. They require infrastructure, multiple resources and interdisciplinary collaboration. The purpose of the center is not to compete with departments and colleges but to be a catalyst to develop programs of research. "The resources that we've developed and made available to our researchers, including the Human Motor Performance laboratories in Jacksonville and Gainesville, are resources that any one department or college might not be able to provide on its own," she adds. The center's resources are further strengthened by close affiliations with the VA Medical Center's Brain Rehabilitation Research Center, led by Leslie Gonzalez Rothi and Stephen Nadeau, and the Rehabilitation Outcomes Research Center, also directed by Duncan. Clinical partnerships with Brooks Health System, Shands Rehabilitation and Shands Jacksonville provide researchers with a large number of patients for clinical trials and the platform to implement the latest research findings into patient care. Duncan says that the Brooks Center's interdisciplinary research is consistent with the National Institutes of Health's emphasis on a team approach and enhances the chances to acquire significant grant awards. The locomotor training that helped Schauble is one example of a research program that has benefited from the Brooks Center. "Before the establishment of the Brooks Center, as an investigator you were a one-stop shop, you did everything yourself. If a wire or a piece of equipment broke, you had to fix it yourself," says Andrea Behrman, who leads the locomotor training research as an associate professor of physical therapy in the College of Public Health and Health Professions. Now rehabilitation researchers have access to bioengineers, statisticians, clinical coordinators, support staff and new equipment. And qualitative researchers who study the consumer's perspective - muscle physiologists, biomechanists, neuropsychologists, neurophysiologists, physical therapists and occupational therapists make up the interdisciplinary research teams. "Improving rehabilitation can't be solved by one person," Behrman says. "Coming together as investigators is so much better than sitting alone, thinking about your corner of the world." Behrman is among a handful of researchers across the country who are studying the use of locomotor training for patients who have experienced a spinal cord injury. By exposing patients to intensive training on a treadmill, researchers hope to activate neural pathways that generate stepping patterns and rebuild the communication between the brain and spinal cord that was damaged during the injury. With funding from the National Institutes of Health, the Christopher Reeve Foundation and the VA Brain Rehabilitation Research Center, Behrman has been working to retrain the legs of patients who still have some function below the level of their spinal cord injury. "Our patients range from those with limited capacity who are using wheelchairs to those who are walking full time, but not so well," Behrman says. "They want to improve balance, endurance, confidence and how they walk - the fine-tuning work." As they walk on the treadmill, patients are partially supported by a specially designed harness. Therapists guide patients' legs and ensure proper gait. The therapy is conducted during one- to two-hour sessions, five days a week for nine weeks.
The intensive training helped Schauble go from a shuffling gait with the assistance of a walker to independent walking with the help of a cane for longer distances. When Schauble began the locomotor training, the harness supported almost all of his body weight. Therapists were stationed at his waist and at each of his arms and legs to guide his body during walking. "The therapists basically retrained me to walk," Schauble says. "When people walk they naturally move the right foot forward and swing the left arm forward at the same time, then the left foot and right arm forward. This is something we learn as infants, but it wasn't automatic for me anymore after the injury." Schauble says the difference the program has made in his life is incredible and he is now back doing many of the things he enjoyed before the injury, including spending time with his grandchildren, even getting up and down from the floor unassisted to join them in play. "My wife and I often talk about what a lucky break this has been for me," Schauble says. "If I had experienced this injury 20 years ago or I lived in a place where the therapy wasn't available, I would have a much different quality of life than I do now." As the participants in the locomotor training program continue to make strides in their recovery, Behrman hopes to understand the parameters of training that will be most effective for patients and answer the questions: Who will benefit from the therapy? When should it be performed, while the patient is still in the hospital or in outpatient therapy? And what intervention is most effective? Behrman says each member of her team contributes to the final result. Steve Kautz, a biomedical engineer, evaluates the biomechanics and mechanisms of changes in gait; Lisa Hannold, a postdoctoral fellow, explores how patient's value the intervention and outcomes; and biostatistician Samuel Wu designs statistical analyses of all new projects. Behrman views her role in the process as a partnership with colleagues and patients, working together to solve the problems of recovery and developing best clinical practices. "Being able to share in this process and see the outcomes is very rewarding, but the process itself is something I value," Behrman says. "I benefit personally from each individual I work with and it intrigues me what each person brings. Although we're trying to come up with a therapy for the masses, spinal cord injury happens to individual people." People like Ernst Kordgien. "I came to UF in a power wheelchair and could use a walker only sparingly," says Kordgien, a 56-year-old middle school principal from Williston, Fla. "Once I got here, we did away with the chair. Then two or three weeks later, the walker went, then my sticks and now I use just a cane, if anything." Andrea Behrman Pamela Duncan Related Web site:
Biomechanics of WalkingSupported by a $1.5 million grant from the National Institutes of Health, Steven Kautz, director of the Brooks and VA human motor performance laboratories, leads a group of clinical researchers and engineers investigating the mechanisms of walking impairment in stroke patients. The laboratories enable researchers to conduct basic science and clinical research with the most comprehensive human movement technology available. Basic ScienceFloyd Thompson of the McKnight Brain Institute is conducting basic science studies of the neurobiology and neurophysiology of walking that will serve as a bridge to human applications of walking therapies. Patient's PerspectiveVA researcher Lisa Hannold is investigating the psychosocial impact of locomotor training. Her previous research has demonstrated that patients value the therapy for the improvement it makes in their walking ability, knowledge gained about ambulation, hope for further recovery and the social support provided by the training team. Outcome MeasurementOccupational therapy investigator Craig Velozo is developing outcome measurement tools that will provide researchers and clinicians with more meaningful evaluations of the effects of treatments on patients' walking ability. Clinical trialsWith funding from an NIH planning grant, Pamela Duncan is leading a team of investigators from UF, UCLA and the University of Southern California in the design of a multi-site clinical trial to evaluate a walking recovery program which includes treadmill training. The trial will be the largest randomized clinical trial of a rehabilitation intervention ever performed. FinancingA health policy research team will examine the cost effectiveness of therapies developed for walking recovery and the economic or health-care system barriers to implementing the treatments.
|