|
|
 Saving FaceUF Maxillofacial Prosthetics Service Rebuilds Faces Damaged by Cancer and Other InjuriesBy Joseph Kays Nancy LuHellier’s dog ate her nose. Luckily for her, University of Florida Anaplastologist Robert Mann can make her a new one. LuHellier’s nose was, and is again, a work of silicone art fashioned by Mann and UF Associate Professor of Prosthodontics Glenn Turner. The two comprise the College of Dentistry’s Maxillofacial Prosthetics Service, where people whose faces are ravaged by cancer, trauma or birth defects come to regain their identity. Two years ago when LuHellier learned a cancerous tumor was going to require surgery that would remove most of her nose, as well as much of her upper palate, she couldn’t imagine joking about it. “I was heartbroken,” says LuHellier, of Hawthorne, Fla. “I couldn’t stand the thought of seeing myself that way.” In fact, for weeks after her surgery, LuHellier was afraid to look at herself in the mirror, and when she did she says she cried for hours. While she was undergoing radiation treatments, LuHellier wore an artificial nose attached to her glasses. “The skin is very sensitive and it has a sunburned tone to it during radiation therapy,” Turner says, “so we don’t do anything permanent until that has healed.” Because the surgery required removal of much of LuHellier’s upper palate, Turner had to create a new upper denture to span the gap. Otherwise, he says, air and food could escape through the opening, making it difficult for her to eat or speak. As part of LuHellier’s denture, Turner fashioned a plastic tab with a magnet about the size of a watch battery on it. This was the anchor for the prosthetic nose Mann would create. Whenever possible, Turner prefers to use implants or magnets in the patient’s face to attach a prosthesis. Another alternative is skin adhesive. “No two surgeries are alike,” says Turner of the prosthodontic techniques he employs depending on the location and extent of the surgery. “We look at what tissue is missing and what we have left to work with and we adapt to each patient.” With her surgery healed, her radiation treatments completed and the denture in place, LuHellier was ready for a new nose. Mann says it takes two full days to create a nose prosthetic from scratch and about three days for an eye with an orbit. Like an artist restoring a canvas, Mann matches the silicone prostheses to the patient’s face, seeking just the right skin tone, then adding details like blood vessels and eyelashes. The work requires great patience on the part of the subject and the artist. Patients likes Robert Seaman, who lost his right eye, must sometimes stare unblinking for hours while Mann puts the finishing touches on a prosthetic to fill the empty socket. Even tiny red blood vessels have been represented in the white of Seaman’s prosthetic eye, making it appear so real that most people would never guess otherwise once it is attached. “Quite often, when patients get their prosthesis they just break down and cry,” Mann says. “I look in the mirror now and know that’s not me,” LuHellier says, “but I can go to town and almost no one else knows it’s not me.” “I was already painting,” he says, “and I was aware of anaplastology, so when I heard about the opportunity at Royal Perth, it seemed like a good opportunity to employ both my dental skills and my art talent.” After working in Australia for several years, Mann eventually made his way to Gainesville, where he teamed up with Turner. While the end result is a work of art, some of the tools of Mann’s trade are amazingly simple.
“Although silicone has none of the properties of real tissue, we try to make it look as much like a patient's own tissue as possible,” Mann says. “We build the effect up in layers, gradually adding color and texture, until we have close to a perfect match.” LuHellier can attest to Mann’s artistic skill. “I have had more people say they never would have known it was not my real nose if I hadn’t told them,” she says proudly. “My family was amazed when they first saw it.” Turner says he decided to specialize in reconstructive dentistry while still in dental school at the University of Alabama and pursued the specialization as soon as he graduated in 1970. He spent five years at a Veterans Administration hospital and stints in private practice and at the University of Kentucky before coming to the University of Florida in 1984.
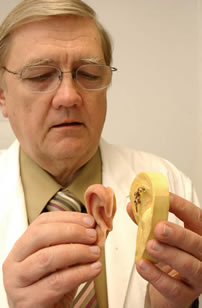
Glenn Turner uses a plaster mold By the early 1980s, doctors at Shands Hospital were doing enough head and neck surgeries to justify an anaplastologist. Today, Turner and Mann treat about 80 patients a year. Turner says that before World War II, there was little recourse for people with disfigured faces, but the many facial wounds the war produced, plus the new synthetic materials that became available, led to dramatic growth in the field. The American Academy of Maxillofacial Prosthetics was founded in 1953 and now has about 270 members. The American Anaplastology Association, organized in 1980, has about 170 members. “We’re a small group. Today there are only about five anaplastologists in the whole state of Florida for 12 million people,” Turner says. “We have people coming from as far away as Georgia and Tennessee.” One of them is George Arnold, who recently got a prosthetic ear to replace the one he lost to cancer three years ago. He says he hasn’t gone anywhere without a hat or a bandage around his head. “You’d be surprised how much a surgery like this can affect you. I got very depressed,” Arnold says. “I sat in my bedroom looking out the window for three years.”
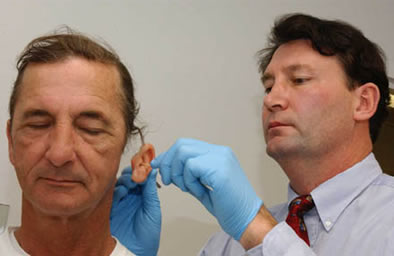
Robert Mann makes some final adjustments to George Arnold's prosthetic Turner and Mann are extremely sensitive to the needs of their patients, and Turner is particularly interested in patients’ quality of life months and years after their surgery. “There are very few support groups for people with head and neck cancers,” Turner says. “We’re interested in how different interventions — including such things as meditation and art therapy — impact quality of life.” Turner recently surveyed about 100 head and neck cancer patients at five sites around the country to determine how their illness has affected their quality of life. Turner hopes results from this pilot study, which was funded with $56,000 from the UF Research Opportunity Fund and $20,000 from the College of Dentistry, will justify funding from the National Institutes of Health for a larger survey. “The results could expand cooperation between prosthodontists, surgeons and physicians and influence how doctors treat different types of head and neck cancers,” Turner says.
Glenn Turner Robert M. Mann
|